A 39 y.o. male comes in with severe epistaxis.
he has frequent nosebleeds. What is his diagnosis?
Our patient had hereditary hemorrhagic telangiectasia (HHT). This is an autosomal dominant genetic condition in which abnormal capillaries form between arteries and veins forming telangiectasias and arteriovenous malformations (AVMs) . Telangiectasia occur on mucous surfaces( lips, GI mucosa ) ; while AVMs occur in solid organs. Hundreds of mutations in several different genes have been linked to HHT. The spectrum of the disease is broad with some people only developing a few telangiectasias later in life and others presenting with nosebleeds in childhood. Clinically, telangiectasia can be distinguished from petechiae since they blanch with pressure and petechiae do not.
The complications of these arterio-venous connections , which are weaker than usual capillaries, include: bleeding, high-output heart failure, brain abscess and Fe deficiency anemia.
40% of patients with HHT have pulmonary avms. The triangle is the avm, the small arrow is the feeding artery and the large arrow is the draining vein.
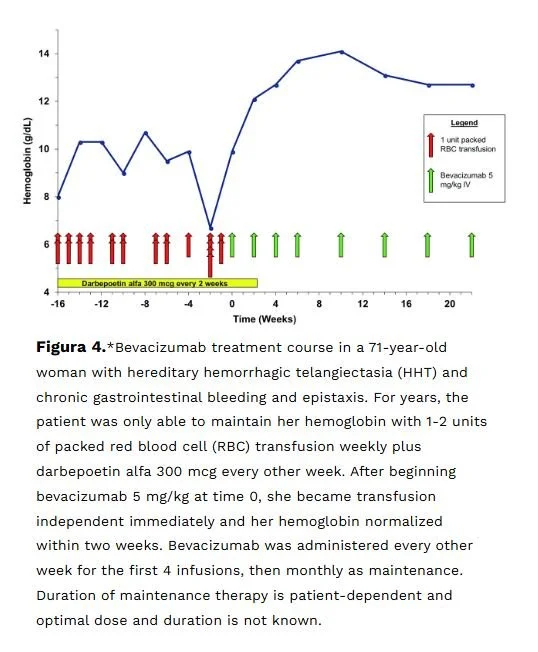
Patients with HHT had high plasma concentrations of transforming growth factor-beta(TGF-beta) and vascular endothelial growth factor (VEGF) Anti-angiogenic agents such as bevacizumab are now being used to treat the disease. They block angiogenesis via VEGF inhibition.
It might be useful to consider the causes of bleeding in general. Consider the following groups.
Genetic abnormalities of blood vessels- HHT, sickle cell disease causing spontaneous hemorrhage by sickled cells causing pressure in the vessels.
Abnormal clotting factors -factors IX, VIII and XIII would be the commonest causing bleeding. Von Willebrands and hemophilia C (factor XI deficiency ) It does not cause spontaneous bleeding but prolonged bleeding after surgery.
Drugs affecting clotting factors or platelets - coumadin , Eliquis, asa, Plavix , SSRIs.
Severe liver disease, causing abnormal clotting factors by decreased production
Antibodies from autoimmune disease-acquired von Willebrands, lupus anticoagulant, antiphospholipid antibodies.
Cancers- systemic mastocytosis can produce heparin causing significant bleeding.
cutaneous mastocytosis in an adult urticaria pigmentosa
FUN FACTS
The condition is also called Osler-Weber-Rendu syndrome after three physicians who independently recognized the disease.
The highest prevalence of HHT is in Afro-Caribbean regions of the Dutch Antilles and France.
Kritharis A , Al-Samkari H, Kuter D. Hereditary hemorrhagic telangiectasia:diagnosis and management from the hematologist’s perspective, Haematologica. 2018. Vol 103 (9)https://doi.org/10.3324/haematol.2018.193003
Westermann CJ, Rosina AF, de Vries V, de Coteau PA. The prevalence and manifestations of hereditary hemorrhagic telangiectasia in the Afro Caribbean population of the Netherlands Antilles: A family screening. Am J of Med Genet. 2003; 116(4):324-328.
D'Souza D, Abu Kamesh M, Campos A, et al. Pulmonary arteriovenous malformation. Reference article, Radiopaedia.org
Lacombe P, Lacout A Marcy P, et al. diagnosis and treatment of pulmonary arteriovenous malformations in hereditary hemorrhagic telangiectasia: an overview. Diagnostic and Interventional Imaging Vol 94(9):835-848,